Recently, we have been faced with a few pertinent questions related to walking as an exercise.
“What is the best time of the day to go on a brisk walk?”
“If I am unable to walk for 30-40 minutes at a stretch, can I break it into small parts?”
“Does walking after a meal have an impact on blood sugar level?”
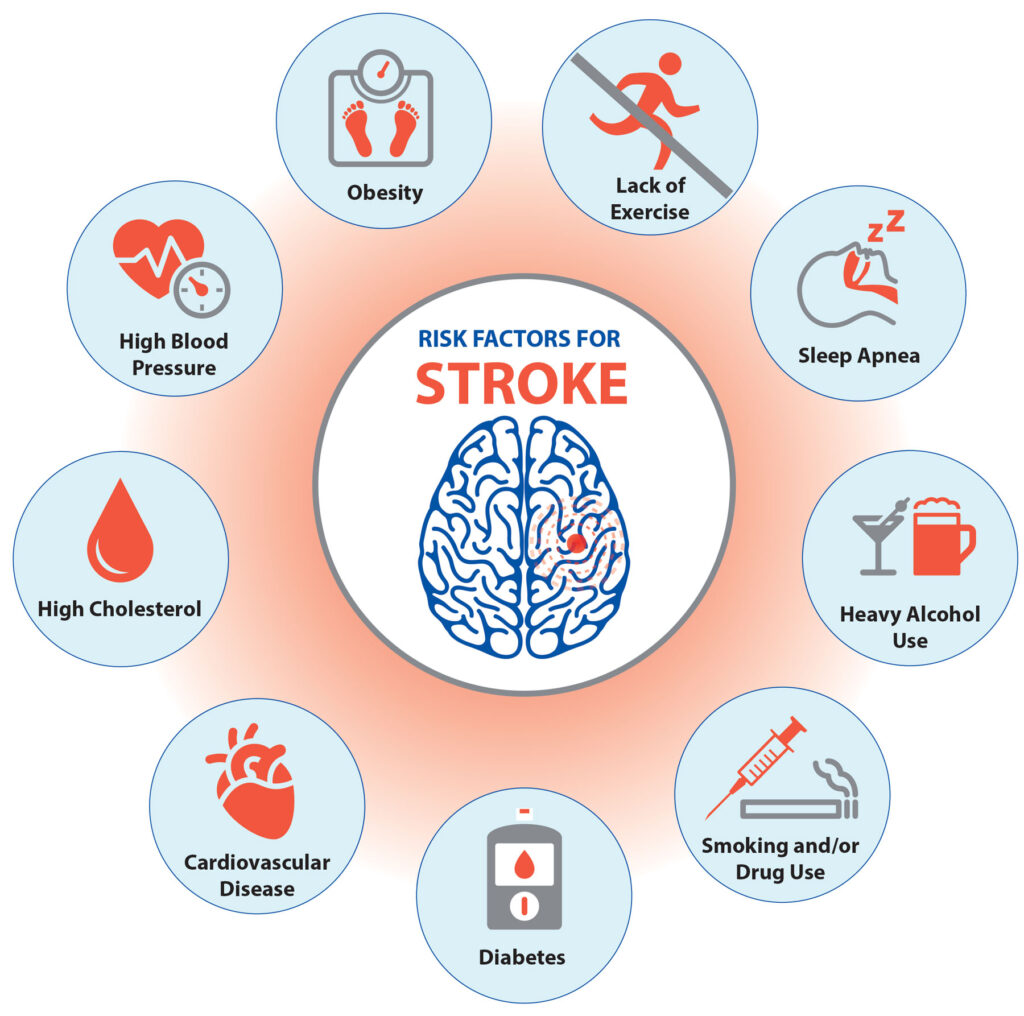
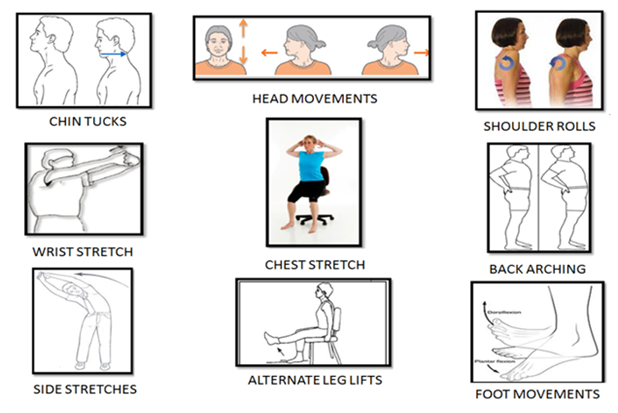
As a team of experts managing individuals with heart diseases and co-morbidities like diabetes, hypertension and obesity, we are pleased to see the growing interest among our people in taking up walking as a form of exercise. We always educate our clients about the importance of warm-up and cool-down exercises as well as the need for a holistic fitness regime which includes muscle strengthening, balance and flexibility components in addition to walking.
The best time of the day to walk
The short answer to this question is there is no one-size-fits-all best time of the day to go for a brisk walk. What is important is the time that works for you as an individual trying to balance family, work, social life and other commitments.
For a mother or father caring for toddlers and young children, it might be the time of the day when the children are sleeping or away at school.
For someone who is working long hours and commuting or traveling frequently, it might be the days of the week that they are not working or working from home.
For those living in locations that have very hot or very cold weather, they may need to find the best time of the day when the temperature is ideal to step out for a walk.

Walking at a stretch versus breaking it down into parts
The maximum benefits of the exercise can be attained by walking for 30 or more minutes at a stretch. However, even short bouts of 10-15 minutes of walking have proven to be beneficial, especially for those who have desk jobs and sit for prolonged periods of time. In fact, walking up and down the stairs a few times at office is an efficient alternative if you are unable to step out. Taking a walking break is the best gift you can give yourself in between those long hours of sitting!
Walking after a meal
According to recent scientific publications, walking after a meal has a greater impact on postprandial glucose levels rather than walking after a few hours after or before a meal. Walking helps the muscles absorb glucose from the bloodstream, which is especially advantageous for people who have diabetes or are at risk of getting it. It can help avoid blood sugar increases after meals, resulting in improved long-term blood sugar control.
Note for heart patients
The important thing to note is that brisk walking or strenuous activity after a meal can pose a threat to heart patients, but gentle walking or taking a stroll after a meal is definitely a good idea. Additionally, focusing on a well-balanced meal instead of a fatty meal is equally important. Please read this related post on balanced meal planning: http://www.cardiacwellnessinstitute.com/heart-disease-treatment-prevention/uncategorized/balanced-diet-vs-crash-diet-for-heart-health/
Other benefits of walking after a meal are:
Aids in digestion:
Your digestion can be aided by movement because it stimulates the stomach and intestines, which allows food to pass through more quickly. Walking can help with bloating, indigestion and heartburns.
Helps with weight management:
We all are aware that walking helps with weight control by burning calories. A little stroll following dinner can be a useful strategy for people trying to maintain or reduce weight. It lessens the accumulation of extra energy as fat and aids in the burning of calories.
Improves quality of sleep:
Walking after dinner puts you in a relaxed state. The more relaxed you are the better is your sleep quality likely to be. Rather than using your mobile phone before sleep, try walking. Remember, there should ideally be at least 2 hours time interval between dinner and hitting the bed.
Improves your mental health:
Taking a stroll following dinner can help you feel more at ease. It’s a chance to unwind, reduce mental stress, and clear your head of worries.
Now that you are enlightened about how best to incorporate walking in your fitness regime, you may start making the necessary changes to your routine right away. If you have been diagnosed with a health condition or have some other concerns, please feel free to get in touch with us (info@cardiacwellnessinstitute.com) or your healthcare provider before embarking on any lifestyle changes.